Introduction
Actinomycosis and actinobacillosis stand out as two intriguing conditions that can affect both humans and animals. While these two infections share similarities, they also possess distinctive characteristics that set them apart.
Understanding the contrasts between actinomycosis and actinobacillosis is vital for the exact conclusion and viable treatment. We’ll dig into the complex points of interest of these contaminations, investigating their side effects, causes, symptomatic strategies, treatment alternatives, and preventive measures. So, let’s embark on this enlightening journey and unravel the unique traits of actinomycosis and actinobacillosis.
Importance of Understanding the Differences between Actinomycosis and Actinobacillosis
Understanding the qualifications between Actinomycosis and Actinobacillosis is of fundamental significance within the field of pharmaceuticals. While these two conditions share certain similarities with bacterial infections, they differ significantly in terms of etiological agents, clinical manifestations, diagnostic approaches, and treatment strategies. By comprehending these differences, healthcare professionals can ensure accurate diagnosis, implement appropriate treatment plans, and improve patient outcomes.
Here are several reasons why understanding the disparities between Actinomycosis and Actinobacillosis is crucial:
1. Accurate Diagnosis: Actinomycosis and Actinobacillosis present with distinct clinical features, and a misdiagnosis can lead to delays in treatment or inappropriate management. By recognizing the specific signs and symptoms associated with each condition, healthcare providers can effectively differentiate between the two and initiate timely interventions.
2. Targeted Treatment: The causative specialists of Actinomycosis and Actinobacillosis, Actinomyces spp. and Actinobacillus spp., respectively, exhibit variations in their susceptibilities to different antimicrobial agents. Understanding these contrasts permits doctors to endorse suitable anti-microbial that successfully target the particular microscopic organisms capable of the disease, driving to way better treatment results and diminished antimicrobial resistance.
3. Management of Complications: Actinomycosis and Actinobacillosis can both give rise to various complications, such as abscess formation, tissue destruction, and dissemination to other body sites. However, the propensity for certain complications may differ between the two conditions. Proper differentiation enables healthcare professionals to anticipate and manage potential complications more effectively.
4. Prognostic Considerations: The prognosis and long-term outcomes of Actinomycosis and Actinobacillosis can vary. Actinomycosis, for instance, may have a chronic and indolent course, requiring prolonged treatment and follow-up. Actinobacillosis, on the other hand, may manifest as an acute infection with a rapid progression. Recognizing these differences aids in providing patients with accurate prognostic information and tailoring appropriate care plans.
5. Public Health Implications: Actinomycosis and Actinobacillosis have implications beyond individual patient care. Understanding the study of disease transmission, courses of transmission, and hazard variables related to these conditions makes a difference in open well-being specialists executing preventive measures, conducting observation, and creating focused intercessions to relieve the spread of these diseases.
Separating between Actinomycosis and Actinobacillosis is vital for precise determination, focused on treatment, administration of complications, the thought of forecast, and open well-being endeavors. By deepening our understanding of the disparities between these conditions, healthcare professionals can provide optimal care, enhance patient outcomes, and contribute to the overall control and prevention of these bacterial infections.
Definition of Actinomycosis and Actinobacillosis
Actinomycosis: Actinomycosis may be an inveterate irresistible illness fundamentally caused by microscopic organisms having a place to the Actinomyces sort. These microbes are filamentous, Gram-positive, anaerobic, or microaerophilic life forms commonly found within the verbal depression, gastrointestinal tract, and female genital tract. Actinomycosis regularly presents as a constant suppurative and granulomatous contamination that can include different anatomical locales, counting the cervicofacial locale, thorax, guts, and pelvis.
Actinobacillosis: Actinobacillosis is an irresistible infection caused by microscopic organisms from the Actinobacillus sort. Actinobacillus species are little, Gram-negative, facultative anaerobic microbes that can be found within the verbal depth, respiratory tract, and regenerative organs of creatures. Contamination with Actinobacillus can happen in both people and creatures, with the last mentioned being more commonly influenced. Actinobacillosis primarily manifests as localized suppurative lesions in the respiratory tract, lymph nodes, or other tissues.
It is imperative to note that whereas Actinomycosis and Actinobacillosis have comparative names and share a few clinical highlights, they are caused by diverse microbes from unmistakable genera. Understanding these microbial distinctions is crucial for accurate diagnosis and appropriate management of these infections.
What is Actinomycosis?
Actinomycosis may be a persistent irresistible illness caused by microscopic organisms from the Actinomyces sort, overwhelmingly Actinomyces israelii. These microscopic organisms are filamentous, Gram-positive, anaerobic, or microaerophilic living beings commonly found within the ordinary vegetation of the verbal depth, gastrointestinal tract, and female genital tract. Actinomycosis typically occurs when these bacteria gain access to deeper tissues following a breach in the mucosal barriers due to trauma, surgery, or other underlying conditions.
Actinomycosis is characterized by the arrangement of abscesses, sinus tracts, and granulomatous injuries that can include different anatomical locales within the body. The foremost common frame of actinomycosis is cervicofacial actinomycosis, which influences the head and neck locale, especially the jaw, mandible, and delicate tissues of the confront. Other sorts of actinomycosis join thoracic actinomycosis (counting the lungs and pleura), stomach actinomycosis (impacting the waist and pelvis), and pelvic actinomycosis (counting the female regenerative organs).
Clinical presentation of actinomycosis can vary depending on the site of infection, but common features include persistent swelling, abscess formation, draining sinus tracts with characteristic sulfur granules (yellowish granules composed of bacterial colonies), and tissue fibrosis. Actinomycosis is frequently slothful and advances gradually, driving the arrangement of incessant, deep-seated abscesses that can include different tissue layers.
Diagnosing actinomycosis requires a combination of clinical doubt, imaging things about such as computed tomography (CT) or attractive reverberation imaging (MRI), and research facility investigation. Microscopic examination of clinical specimens or tissue biopsies may reveal the characteristic branching filaments of Actinomyces organisms, and cultures can be performed to isolate and identify the bacteria. Atomic procedures such as polymerase chain response (PCR) may too help within the recognizable proof of Actinomyces species.
Treatment of actinomycosis ordinarily includes a delayed course of anti-microbial treatment, regularly with high-dose penicillin or other beta-lactam anti-microbials. Surgical intercession may be fundamental to deplete abscesses or expel contaminated tissue. With fitting treatment, the guess for actinomycosis is for the most part favorable, even though long-term follow-up may be required to guarantee total determination of the infection.
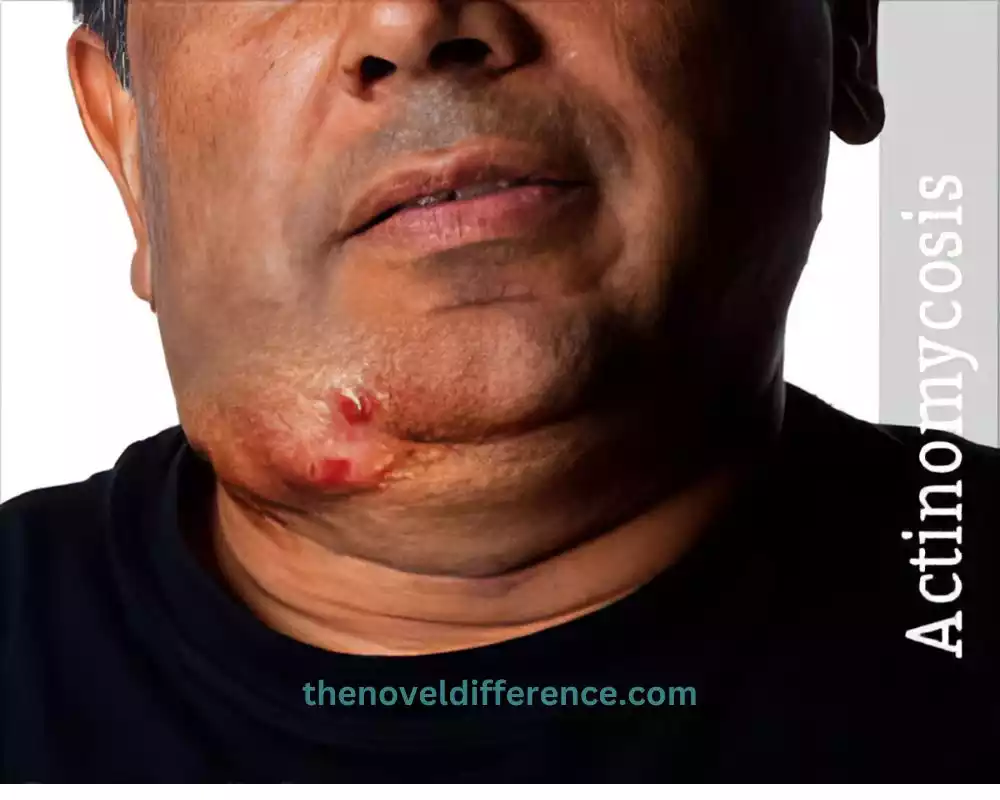
Actinomycosis may be an incessant irresistible malady caused by Actinomyces microbes, characterized by the arrangement of abscesses, sinus tracts, and granulomatous injuries in different anatomical destinations. Prompt diagnosis and appropriate treatment with antibiotics are crucial for managing actinomycosis effectively and achieving favorable outcomes for affected individuals.
Causative agent (Actinomyces spp.)
Actinomycosis, as the title proposes, is essentially caused by microscopic organisms having a place in the Actinomyces class. Actinomyces spp. are filamentous, Gram-positive bacteria that typically have a branching, filamentous appearance. The first common species included in actinomycosis is Actinomyces israelii, but other species interior the Actinomyces lesson, such as Actinomyces naeslundii, Actinomyces viscous, and Actinomyces odontolyticus, can as well be included.
These microscopic organisms are a portion of the typical greenery of the verbal depth, gastrointestinal tract, and female genital tract in people. They exist as commensal organisms, usually without causing any harm. However, when there is a breach in the mucosal barriers due to trauma, surgery, or underlying conditions such as dental caries, periodontal disease, or foreign body presence, Actinomyces can invade the surrounding tissues and cause infection.
The ability of Actinomyces to form biofilms and their resistance to phagocytosis contributes to their pathogenicity. Once they establish infection, Actinomyces bacteria can create chronic, suppurative lesions characterized by abscesses, sinus tracts, and granulomatous inflammation.
It’s worth noting that while Actinomyces spp. are the primary causative agents of actinomycosis, there have been rare cases where other bacteria, such as Nocardia spp. or other filamentous bacteria, have been implicated as the causative agents. However, Actinomyces species remain the most common etiological agents of actinomycosis.
Transmission and risk factors
Actinomycosis isn’t an infectious illness and does not spread from individual to individual. Instead, it typically occurs when Actinomyces bacteria, which are part of the normal flora, gain access to deeper tissues following a breach in the mucosal barriers.
The transmission and risk factors associated with actinomycosis can be attributed to various factors:
1. Endogenous Infection: Actinomyces bacteria reside in the oral cavity, gastrointestinal tract, and female genital tract of humans as commensal organisms. The bacteria can cause infection when they invade tissues due to trauma, dental procedures, surgical interventions, or underlying conditions that disrupt the mucosal barriers. Poor oral hygiene, dental caries, periodontal disease, and dental abscesses increase the risk of Actinomyces infection in the cervicofacial region.
2. Foreign Body Presence: Actinomycosis can develop when Actinomyces bacteria colonize foreign bodies, such as intrauterine devices (IUDs), dental appliances, or surgical implants. These foreign objects can serve as a nidus for bacterial growth and facilitate the establishment of infection.
3. Associated Conditions: Certain underlying conditions or comorbidities can predispose individuals to actinomycosis. For instance, chronic alcoholism, immunodeficiency disorders, poorly controlled diabetes mellitus, malnutrition, and malignancies can weaken the immune system, making individuals more susceptible to Actinomyces infection.
4. Invasive Procedures: Invasive medical procedures, such as surgeries, colonoscopies, or endoscopic interventions, may disrupt the mucosal barriers and provide an opportunity for Actinomyces bacteria to invade deeper tissues. This can lead to postoperative or post-procedural actinomycosis.
5. Gender and Age: A few things about recommend the next rate of actinomycosis in guys compared to females, particularly for certain sorts of actinomycosis like thoracic or stomach inclusion. Age can too be a figure, with cervicofacial actinomycosis being more common in more youthful people and other shapes of actinomycosis, such as thoracic or stomach, being more predominant in more seasoned people.
It is imperative to note that Actinomyces spp. is a portion of the ordinary vegetation, and the nearness of these microbes alone does not essentially demonstrate disease or infection. The development of actinomycosis requires specific predisposing factors that enable the bacteria to breach mucosal barriers and invade deeper tissues.
Understanding the transmission and chance components related to actinomycosis can offer assistance to healthcare experts distinguish people at higher chance, consider fitting preventive measures, and keep up a tall record of the doubt for the malady in helpless populaces.
What is Actinobacillosis?
Actinobacillosis is an irresistible malady caused by microscopic organisms from the Actinobacillus sort. Actinobacillus species are little, Gram-negative, facultative anaerobic microbes that can be found within the verbal depression, respiratory tract, and regenerative organs of creatures. While primarily affecting animals, actinobacillosis can also occur in humans, albeit rarely.
Actinobacillus contamination is more predominant and can influence different species, counting cattle, pigs, sheep, and steeds. The bacteria can cause localized suppurative lesions, abscesses, or systemic infections in affected animals. The foremost common frame of actinobacillosis in creatures is the respiratory frame, which shows pneumonia, pleuritis, or lymphadenitis.
Actinobacillosis is a rare infection, and cases are usually associated with occupational exposure to animals or animal products. People who work with creatures, such as ranchers, veterinarians, or abattoir laborers, maybe a higher chance. The disease regularly happens through coordinated contact with sullied materials, such as creature chomps, scratches, or inward breath of respiratory discharges.
Actinobacillosis in humans usually presents as localized infections, most commonly affecting the head and neck region. Cervicofacial actinobacillosis, characterized by abscess formation, lymphadenopathy, and tissue swelling, is the most frequently reported form in humans. However, other forms, such as pulmonary or systemic involvement, can occur, albeit less frequently.
Diagnosing actinobacillosis includes a combination of clinical assessment, imaging thinks about, and research facility testing. Minuscule examination of clinical examples or tissue biopsies may uncover the nearness of Gram-negative coccobacilli, and societies can be performed to confine and distinguish the Actinobacillus species included. Molecular techniques, such as PCR, can aid in species identification.
Treatment of actinobacillosis customarily incorporates antimicrobial treatment, such as penicillin or other beta-lactam anti-microbials. Surgical drainage or debridement may be necessary for abscesses or extensive tissue involvement.
Prevention of actinobacillosis primarily focuses on implementing appropriate hygiene measures and avoiding direct contact with animals or animal products, especially in occupational settings.
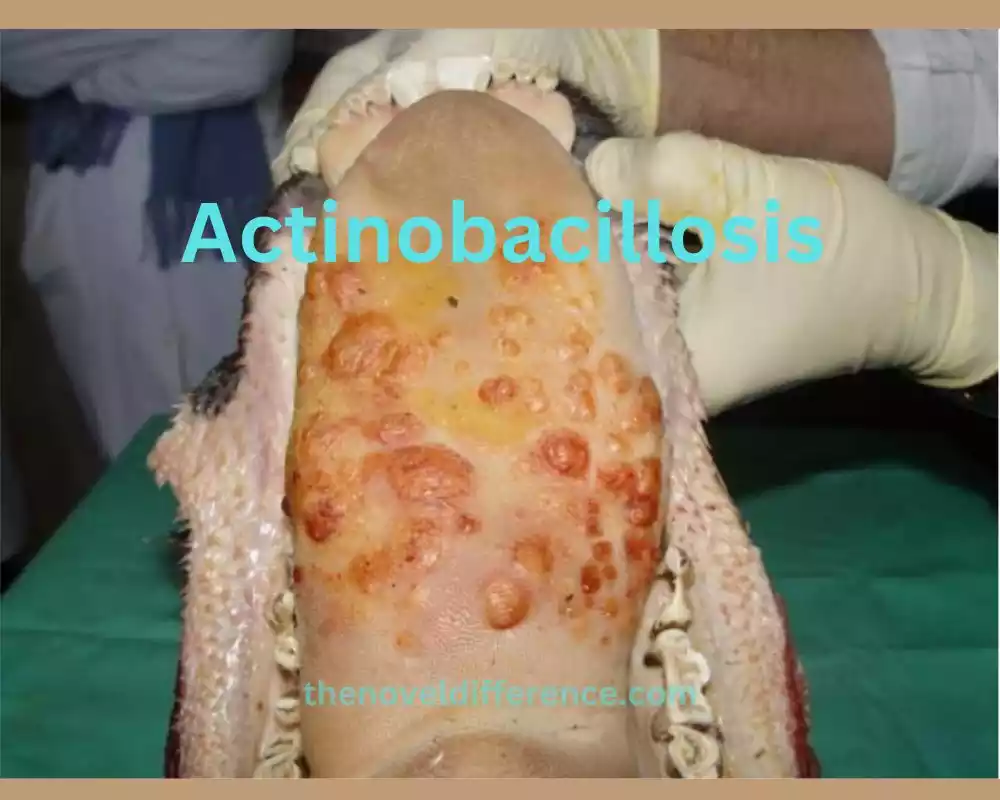
Whereas actinobacillosis could be an uncommon disease in people, it is critical to consider the plausibility, particularly in people with a word-related introduction to creatures. Prompt diagnosis and appropriate treatment are essential for managing actinobacillosis effectively and preventing complications.
Causative agent (Actinobacillus spp.)
Actinobacillosis, as the title recommends, is fundamentally caused by microbes from the Actinobacillus sort. Actinobacillus spp. are little, Gram-negative, facultative anaerobic microscopic organisms that can be found within the verbal depth, respiratory tract, and regenerative organs of creatures. The most common species implicated in actinobacillosis is Actinobacillus lignieresii, also known as Trueperella pyogenes.
Actinobacillus lignieresii is a normal inhabitant of the mucous membranes in the oral cavity of animals, particularly ruminants like cattle and sheep. The bacteria can cause infection when they gain access to deeper tissues through breaches in the mucosal barriers, such as mucosal erosions, traumatic injuries, or contaminated wounds.
It’s imperative to note that Actinobacillus species can too cause other diseases in creatures, such as respiratory diseases, septicemia, or regenerative tract contaminations. Actinobacillus diseases, counting actinobacillosis, are generally uncommon and regularly related with word-related introductions to creatures or creature items.
The pathogenicity of Actinobacillus species is credited to their capacity to create different harmfulness variables, such as adhesins, poisons, and chemicals, which contribute to tissue intrusion and the advancement of localized suppurative injuries.
Actinobacillus species, fundamentally Actinobacillus lignieresii, are the causative operators of actinobacillosis. These bacteria are part of the normal flora of animals, particularly ruminants, and can cause infection when they breach mucosal barriers and invade deeper tissues. Proper diagnosis and targeted treatment are necessary for managing actinobacillosis effectively in both animals and, although rare, in humans.
Transmission and risk factors
Actinobacillosis is primarily an infectious disease of animals, but it can rarely affect humans. The transmission and chance variables related to actinobacillosis are affected by the characteristics of the causative microscopic organisms (Actinobacillus spp.) and the presentation to sullied materials.
Here are the key points regarding transmission and risk factors:
Transmission in Animals:
1. Direct Contact: Actinobacillus bacteria are primarily transmitted among animals through direct contact. This can occur through bites, scratches, or proximity to infected individuals.
2. Ingestion: Ingesting contaminated food or water can also contribute to the transmission of Actinobacillus bacteria among animals.
3. Opportunistic Infections: Actinobacillosis often occurs as opportunistic infections when the animal’s immune system is compromised due to underlying conditions, stress, or concurrent diseases.
Risk Factors in Animals:
1. Animal Husbandry: Animals kept in crowded or unhygienic conditions, such as farms or feedlots, are at a higher risk of exposure to Actinobacillus bacteria.
2. Trauma: Wounds or injuries in animals, especially those involving the oral cavity or respiratory tract, provide an entry point for Actinobacillus bacteria.
3. Immunodeficiency: Animals with weakened immune systems, whether due to genetic factors, stress, or other diseases, are more susceptible to Actinobacillus infections.
Transmission to Humans:
1. Occupational Exposure: Humans who work closely with animals, such as farmers, veterinarians, or abattoir workers, may be at a higher risk of contracting actinobacillosis. Direct contact with infected animals, animal bites, or exposure to contaminated materials can lead to infection.
2. Inhalation: Inhalation of respiratory secretions or aerosolized particles from infected animals can potentially transmit Actinobacillus bacteria to humans.
Risk Factors in Humans:
1. Occupational Exposure: People who are in constant contact with animals, specifically those who are involved in handling animals or veterinary treatment are at greater risk chance of contracting actinobacillosis.
2. Immunocompromised Individuals: People with compromised immunity due to medical conditions or taking immunosuppressant treatments are more prone to contracting Actinobacillus.
Remind yourself that although actinobacillosis may affect humans, its incidence tends to be rare and usually linked with occupational exposures or close contact with affected animals. Implementing appropriate hygiene practices, maintaining good wound care, and following safety protocols when working with animals can help reduce the risk of transmission to both animals and humans.
Differences between Actinomycosis and Actinobacillosis
Actinomycosis and actinobacillosis are two distinct infectious diseases caused by different bacteria and affecting different species.
Here are the key differences between actinomycosis and actinobacillosis:
1. Causative Agents:
• Actinomycosis: Actinomycosis is primarily caused by bacteria from the Actinomyces genus, predominantly Actinomyces israelii. Actinomyces family species such as Actinomyces naeslundii (Antinom) or Actinomyces odontolyticus could also play a part in disease treatments, particularly when employed to clean dental plaque or tartar deposits.
• Actinobacillosis: Actinobacillosis is caused by bacteria from the Actinobacillus genus, most commonly Actinobacillus lignieresii (Trueperella pyogenes).
2. Species Affected:
• Actinomycosis: Actinomycosis can affect both animals and humans. Cervicofacial Actinomycosis is the most prevalent type, while others can include abdominal, thoracic, and pelvic manifestations.
• Actinobacillosis: Actinobacillosis primarily affects animals, including cattle, pigs, sheep, and horses. It can rarely occur in humans, usually associated with occupational exposure to animals or animal products.
3. Mode of Transmission:
• Actinomycosis: Actinomyces bacteria are part of the normal flora and typically cause infection when they gain access to deeper tissues through breaches in the mucosal barriers, such as trauma, surgery, or underlying conditions.
• Actinobacillosis: Actinobacillus bacteria are transmitted among animals through direct contact, such as bites, scratches, or proximity. In humans, occupational exposure to infected animals or contaminated materials can lead to transmission.
4. Clinical Presentation:
• Actinomycosis: Actinomycosis is characterized by the formation of abscesses, sinus tracts, and granulomatous lesions in various anatomical sites. The clinical presentation depends on the site of infection but often includes persistent swelling, abscess formation, draining sinus tracts, and tissue fibrosis.
• Actinobacillosis: Actinobacillosis in animals typically presents as localized suppurative lesions, abscesses, or systemic infections. In humans, it most commonly manifests as cervicofacial actinobacillosis, characterized by abscess formation, lymphadenopathy, and tissue swelling.
5. Treatment:
• Actinomycosis: Treatment of actinomycosis involves a prolonged course of antibiotic therapy, usually with high-dose penicillin or other beta-lactam antibiotics. Surgical intervention may be necessary in some cases to drain abscesses or remove infected tissue.
• Actinobacillosis: Actinobacillosis in animals is often treated with antimicrobial therapy, such as antibiotics effective against Actinobacillus species. Treatment in humans may involve antibiotic therapy and, if necessary, surgical drainage or debridement.
An understanding of these differences between them is paramount for accurate diagnosis, effective treatments, and management of both actinomycosis and actinobacillosis. It highlights the importance of considering the specific causative agents and target species when dealing with these infectious diseases.
Similarities between Actinomycosis and Actinobacillosis
Actinomycosis and Actinobacillosis are distinct infections caused by different species of bacteria; nonetheless, both may share similarities in terms of the infection process and symptoms.
Both may share certain similarities as well:
1. Bacterial Infections: Actinomycosis and Actinobacillosis are bacteria-related infections caused by Gram-negative bacteria; respectively Actinomycosis may be due to bacteria belonging to Actinomyces Genus while Actinobacillosis could be Actinobacillus Genus bacteria.
2. Opportunistic Infections: Both diseases often occur as opportunistic infections. They typically take advantage of compromised host defenses or breaches in mucosal barriers to establish an infection. In Actinomycosis, Actinomyces bacteria invade deeper tissues following trauma, surgery, or underlying conditions. In Actinobacillosis, Actinobacillus bacteria infect animals when there is direct contact, bites, or scratches.
3. Abscess Formation: Both diseases can lead to the formation of abscesses. Actinomycosis is known for the development of chronic abscesses with characteristic sulfur granules. Actinobacillosis can also result in localized suppurative lesions and abscess formation, particularly in animals.
4. Clinical Presentations: Although the clinical presentations differ based on the affected species and anatomical sites, both diseases can cause localized tissue swelling, abscesses, and lymphadenopathy. Cervicofacial involvement is common in both Actinomycosis and Actinobacillosis.
5. Treatment Approach: The treatment approaches for both diseases involve a combination of antimicrobial therapy and, in some cases, surgical intervention. Antibiotics are effective against the respective causative bacteria and are used to target the infections. Surgical drainage or debridement may be necessary to manage abscesses or remove infected tissue.
While there are these similarities, it is important to note that the causative bacteria, species affected, modes of transmission, and specific clinical manifestations differ between Actinomycosis and Actinobacillosis. Understanding these similarities and differences is crucial for accurate diagnosis, appropriate treatment, and optimal management of the respective infections.
Conclusion
Actinomycosis and actinobacillosis are distinct bacterial infections with unique characteristics, affecting both humans and animals. By understanding the differences between these infections, including their causes, clinical presentations, diagnostic approaches, treatment modalities, and preventive measures, we can ensure timely intervention and improve patient outcomes.
By taking care to address medical needs and taking preventive steps early, the effects of both actinomycosis and actinobacillosis could potentially be reduced. Stay informed, maintain good hygiene practices, and consult healthcare professionals or veterinarians for prompt diagnosis and treatment.
