Hemangioma and Vascular Malformation, Hemangiomas are a category of vascular abnormalities that affect people of all ages. They both cause abnormalities of blood vessels but they are different in their causes, characteristics, and management.
This brief introduction will examine the differences between benign vascular tumors (hemangiomas) and congenital structural abnormalities (vascular malformations), shedding light on the importance of these two conditions in healthcare.
What is Hemangioma?
Hemangioma, a type of vascular abnormality, is characterized by an abnormal growth of blood vessels in the body. This benign (noncancerous), non-cancerous tumor usually develops within the first weeks or months of life. Hemangiomas may occur anywhere on your body but are more common on the skin. They can be found most often on the head, neck, and face.
Hemangiomas have the following characteristics:
- Proliferative phase: Hemangiomas go through rapid growth soon after they appear. This phase can cause concern for parents and caregivers as the tumor’s size may rapidly increase.
- Involutive phase: Most hemangiomas shrink over time after the proliferative stage. This process may take several years, and it can result in the complete disappearance of the hemangioma.
- Appearance: Hemangiomas have a variety of appearances. The nodules may be raised, pink, or red. Some have a bluish color or texture that resembles a strawberry, hence the name “strawberry hemangiomas”. The color and texture can change as they involute.
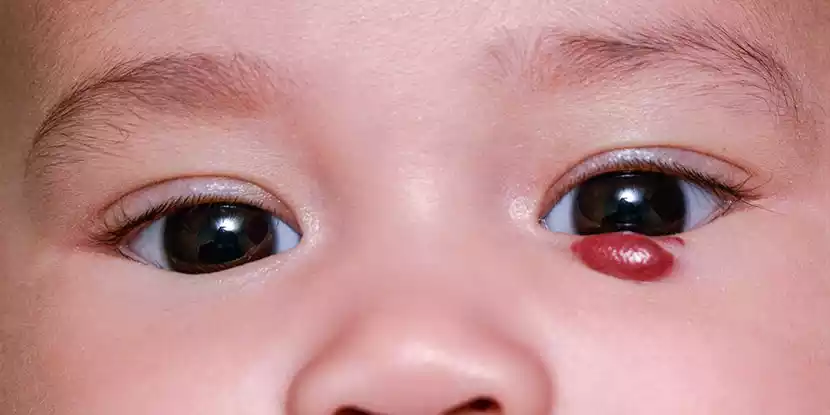
Hemangiomas do not usually appear at birth, but they develop soon after. Their rapid growth, appearance, and location can be concerning, especially if the hemangiomas affect vital organs or structures. Most hemangiomas don’t require treatment as they usually resolve themselves over time. Medical or surgical intervention may be required in some cases, especially when there are functional or medical issues.
What is Vascular Malformation?
A vascular abnormality is characterized by malformed, abnormal blood vessels. These malformations are present at birth and can persist for the rest of one’s life. Contrary to hemangiomas which are benign tumors, vascular malformations affect the structure of blood vessels. These malformations may affect different parts of the human body including the skin and muscles.
The following are the key characteristics of vascular malformations:
- Congenital: Vascular Malformations can be present at birth, and they may get more noticeable as the person grows. However, they don’t proliferate like hemangiomas.
- Abnormal vessel development: These anomalies are caused by errors in the development of blood vessels during embryonic growth. These anomalies can affect capillaries as well as veins, lymphatic vessels, or arteries.
- Categorization: Vascular malformations can be classified into several types depending on which blood vessels are affected. Common types include:
- Capillary malformations: These are capillary malformations, also known as port wine stains. They often appear as birthmarks that are red or purple.
- Venous malformations: These can cause swollen or bluish areas of the skin.
- Lymphatic malformations: These malformations, involve lymphatic vessels and can lead to fluid-filled cysts and masses.
- Arteriovenous malformations (AVMs): Abnormal connections of arteries and veins that can cause blood flow problems or tissue damage.
The size and severity of vascular malformations can vary, as well as their clinical presentation depending on where they are located. Some vascular abnormalities are small and do not cause symptoms, but others can cause pain, functional impairment, and complications.
Diagnostics of vascular malformations usually involve a clinical examination by a healthcare provider, as well as imaging studies like computed tomography scans (CT), angiography, and magnetic resonance imaging to determine the extent of the malformation. In some cases, genetic testing is necessary, particularly if there’s a family history.
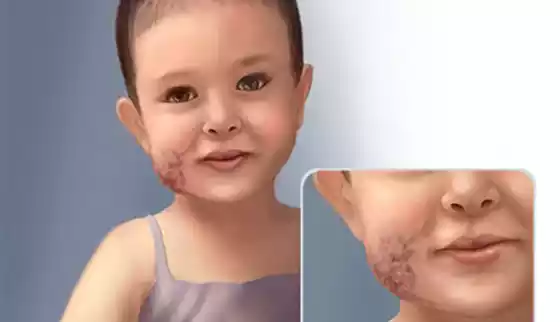
The type, location, and severity of a vascular malformation will determine the treatment options. Treatment options include conservative management (such as embolization and sclerotherapy) or surgical interventions that remove or repair abnormal vessels. Treatment is tailored to each patient’s specific needs, as well as the risks and benefits of each treatment option.
For individuals with vascular abnormalities, it’s important to consult a medical expert, such as an interventional radiologist or vascular surgeon, to receive the proper diagnosis and treatment. Early intervention may help relieve symptoms and reduce complications in certain cases.
What causes hemangiomas and Vascular Malformations?
Hemangiomas, vascular malformations, and vascular anomalies are different types of vascular abnormalities with distinct underlying causes. Here is a brief overview of each type:
Hemangiomas: result from abnormal development of blood vessels during fetal growth and are not usually present at birth. Hemangiomas are not completely understood. However, research indicates that genetic and environmental factors could play a part.
Some possible contributing factors include:
- Genetic predisposition: Hemangiomas can run in families.
- Factors of Hormones: Changes in hormones during pregnancy can influence the growth of hemangiomas. They are more common among female infants or premature infants.
- Immune system: According to some researchers, the immune system could play a part in the growth and evolution of hemangiomas.
- Environmental Triggers: Although not conclusively proven, certain environmental factors, or maternal behaviors, such as drug or smoking use during pregnancy, have been suggested as possible contributors.
Malformations Vasculaires: Malformations vasculares are present at birth, and they result from embryonic errors. These are not tumors, like hemangiomas, but structural abnormalities of the blood vessels. These include:
- Genetic Mutations: In certain cases, genetic mutations can be responsible for the development of vascular malformations. These mutations may affect genes that are involved in the formation of blood vessels.
- Embryonic development: Vascular Malformations are caused by the incorrect formation of blood vessels during the fetal stage. This can cause a variety of malformations including capillary malformations and venous, arteriovenous, or lymphatic malformations.
- Spontaneous occurrence: Vascular malformations can occur without any known genetic or environmental trigger.
While there are likely to be environmental or genetic factors involved in the development of hemangiomas, the causes must vary from person to person. Research in this area continues and may lead to new insights in the future. Medical specialists are usually needed to diagnose and manage these conditions. They can tailor a treatment plan based on each patient’s needs and condition.
Hemangioma and Vascular Malformation in Tabular Form
Here’s a comparison of Hemangioma and Vascular Malformation in tabular form:
| Aspect | Hemangioma | Vascular Malformation |
|---|---|---|
| Nature | Benign vascular tumor | Structural abnormalities in blood vessels |
| Congenital vs. Acquired | Typically not present at birth; develops shortly after birth | Present at birth; congenital |
| Growth | Rapid growth during the proliferative phase followed by gradual involution | Generally stable in size and structure throughout life |
| Types | Not categorized by vessel type; may involve multiple vessel types | Categorized into various types (e.g., capillary, venous, lymphatic, arteriovenous) based on the affected blood vessels |
| Clinical Presentation | – Red or pink nodules on the skin, often raised during the proliferative phase – Change in color and texture as they involute | – Red, purple, or bluish discolorations on the skin (depending on type) – Swelling or fluid-filled cysts in some cases |
| Onset | Usually appears shortly after birth or within the first few weeks of life | Present at birth and persist throughout life |
| Causes | Not fully understood; may involve genetic and environmental factors | Result from errors in embryonic vascular development; may have genetic factors |
| Treatment | – Observation – Medical therapy (if necessary) – Surgical intervention (if complications or functional issues arise) | – Conservative management – Interventional procedures (e.g., embolization, sclerotherapy) – Surgical treatment (for extensive or problematic malformations) |
| Prognosis | Typically favorable; most involute and resolve without treatment | Variable, depending on the type, size, and location; some may remain stable while others can cause complications |
| Diagnosis | – Clinical evaluation – Imaging techniques (e.g., ultrasound, MRI) – Histopathology (if needed) | – Clinical evaluation – Imaging (e.g., MRI, CT, angiography) – Genetic testing (if applicable) |
| Common Locations | Face, neck, head, or any part of the body | Skin, muscles, bones, internal organs |
| Management | Often managed by pediatricians or dermatologists | Typically requires specialized care from vascular specialists (e.g., vascular surgeons, interventional radiologists) |
Please note that the specific characteristics and management of these conditions can vary depending on the individual case and the type of vascular malformation involved. Consultation with a medical specialist is crucial for accurate diagnosis and appropriate management.
What should I do if my child has a hemangioma or other forms of vascular malformations?
If your child has a hemangioma or other vascular malformation, you should take the following measures to ensure that it is properly evaluated, managed, and treated:
- Consult with a Medical Expert: Seek the help of a healthcare provider who is an expert in vascular anomalies. You may need to consult a dermatologist or pediatric dermatologist. A pediatric surgeon, vascular specialist, interventional radiologist, or pediatrician will also be needed depending on the severity and location of the condition. They will evaluate the condition and advise on the best course.
- Accurate Diagnoses: Confirm diagnosis by clinical evaluation, and if needed, imaging studies, such as CT scans, MRIs, CTs, or angiography. A correct diagnosis is essential for determining the best management plan.
- Understanding the Condition: Find out as much as possible about the type of vascular abnormality your child has. This includes its characteristics, any potential complications, and treatment options. Understanding the condition can help you make informed choices and advocate for your child.
- Create a Treatment Plan: Work with your medical specialist to create a treatment plan that is tailored to the needs of your child. Treatment options include medical therapy, surgical intervention, or interventional procedures such as embolization and sclerotherapy. Treatment options will vary depending on the size, type, and location of the vascular abnormality, as well as any symptoms or complications.
- Regular follow-up: Adhere to the treatment plan and follow the recommended schedule for regular check-ups. Regular monitoring is necessary to monitor the progression of vascular anomalies and make adjustments as needed.
- Psychological support: A diagnosis of a vascular abnormality can be emotionally challenging for you and your child. You can seek emotional support from friends, family members, or groups that specialize in vascular abnormalities. If you need to cope with emotional or psychological stress, consider counseling or therapy.
- Educate Others: Make sure family members, teachers, and caregivers are aware of your child’s illness so they can provide the best care.
- Advocate For Your Child: Be a champion for your child’s health care needs. Ask questions, get second opinions, if needed, and make sure your child gets the best care possible.
- Be prepared for changes: Vascular abnormalities can change, and treatment plans might need to be adjusted. Be prepared to adjust your treatment plan if necessary.
- Support Organizations: Investigate support groups and patient advocacy organizations dedicated to vascular abnormalities. These organizations provide families with valuable resources and information. They can also help them feel a part of a community.
Each case of hemangioma, or vascular malformation, is unique. The management approach will differ based on specific circumstances. Consult a healthcare professional who has experience in treating vascular abnormalities to ensure your child gets the right care.
Case Studies and Examples
Case studies and examples can be powerful tools to illustrate key concepts and practical applications in various fields including medicine.
Below are some brief examples of hemangiomas or vascular malformations:
Case Study 1: Hemangioma:
Patient profile: Sarah is a 6-week-old infant who presented with a bright red nodule rapidly growing on her forehead.
Clinical Presentation: Sarah’s parents first noticed the lesion soon after Sarah was born. It had also grown over the last few weeks. It was red and raised with a strawberry appearance.
Diagnosis: Following a clinical examination and ultrasound imaging, Sarah was diagnosed as having an infantile haemangioma.
Treatment: Due to the size and location of her hemangioma, her pediatrician advised close observation and explained to her parents infantile hemangiomas can involute themselves. The parents were told to keep an eye on it and make follow-up appointments.
Case Study No. 2: Vascular Malformation:
Patient profile: Mark is a 16-year-old teenager who has experienced swelling and pain in his left leg.
Clinical presentation: Mark experienced episodes of swelling and pain in his leg that were especially concerning when he was physically active. The left leg was also larger than the right.
Diagnosis: The clinical evaluation and imaging (MRI), revealed a venous abnormality in Mark’s leg.
Treatment: Mark’s case was discussed by a vascular specialist, who recommended an interventional treatment. Sclerotherapy was performed to reduce the size of the vein malformation and improve its symptoms. His progress was monitored by regular follow-up appointments.
Examples of Importance: The case studies in this article highlight the importance that accurate diagnosis plays in determining the best course of treatment for patients who have vascular anomalies. Sarah’s early diagnosis of a hemangioma infantile allowed her to be observed and comforted by her parents. Mark’s diagnosis of vein malformation was timely, which allowed for targeted treatment to relieve symptoms and improve quality of life.
These examples show how an accurate diagnosis followed by the appropriate management or treatment can result in better outcomes for people with hemangiomas or vascular malformations.
Importance of Accurate Diagnosis
For many reasons, accurate diagnosis is crucial in healthcare, including for conditions such as hemangiomas, vascular malformations, and other medical conditions.
Below are some key reasons that highlight the importance of an accurate diagnosis:
- Selecting the Right Treatment: A correct diagnosis is essential to selecting the best treatment plan or management strategy. A correct diagnosis is essential to determining the best course of treatment for different medical conditions. Treatment options for vascular anomalies can range from simple observation to complicated surgical procedures. The choice is dependent on the diagnosis.
- Complications Prevention: If not managed properly, many medical conditions, such as vascular anomalies can cause complications. A correct diagnosis can allow for early intervention to prevent or minimize potential complications. Early treatment of arteriovenous (AVM) malformations can, for example, prevent organ damage or serious bleeding.
- Best Use of Resources: The resources available for healthcare, such as time, personnel, and finances, are limited. Accurate diagnosis allows for efficient resource allocation. When the right condition is diagnosed, unnecessary tests, treatments, or hospitalizations are avoided, which reduces healthcare costs and side effects.
- Patient Safety and Well-being: Accurate diagnoses are fundamental for patient safety. A delayed or incorrect diagnosis can result in wrong treatments, unnecessary pain, and even harm to patients. Assuring that the correct diagnosis is made is an important aspect of patient care.
- Patient education and informed decision-making: Patients and their families can make better decisions when they have an accurate diagnosis. They will be able to understand their condition and the treatment options available. Well-informed patients can take an active role in making healthcare decisions. They can make choices that reflect their values and preferences.
- Research & Advancements: Accurate diagnosis contributes to medical research and advancement of medical knowledge. Researchers depend on accurate diagnosis to understand epidemiology, develop new treatments, and improve existing ones.
- Legal Considerations and Ethics: Accurate diagnosis is crucial in ethical and legal contexts. These diagnoses can have a significant impact on insurance claims, disability determinations, and legal liability. Fairness and justice require accurate diagnoses.
- Public Health & Epidemiology: Accurate diagnosis is essential to tracking the prevalence and incidence of diseases in populations. Accurate data is essential for public health authorities to plan and implement interventions such as vaccinations or disease surveillance.
- The Quality of Life: An accurate diagnosis can have a significant impact on an individual’s life quality. This can result in a quicker relief of symptoms and an improved overall feeling of well-being. It can even save lives in some cases.
- Avoiding unnecessary Stress: A wrong diagnosis can cause stress and anxiety to patients and their family members. This can lead to unnecessary treatment or medication with side effects.
Accurate diagnosis is at the core of good healthcare. It is important to ensure that patients are receiving the right care, promote patient safety, and contribute to the well-being of both individuals and populations. To achieve the best outcomes, healthcare professionals, patients, and the entire healthcare system must place a high priority on the accuracy of diagnosis.
Conclusion
Accurate diagnosis is essential to effective healthcare. It allows for appropriate treatment, prevents complications, ensures patient safety, and empowers informed decision-making. It is crucial to improving the quality of care and patient outcomes.
