Alteplase and Streptokinase are both thrombolytics used to dissolve blood clots. Both have the same essential function, which is to dissolve blood clots. However, their mechanisms of action, clinical indications, and safety profiles are very different.
It is important that healthcare professionals understand the differences between the two drugs to be able to make an informed decision when choosing the best thrombolytic treatment for their patients. This brief introduction will give a quick overview of Streptokinase, and Alteplase before we delve into their differences in greater detail.
Brief overview of thrombolytic agents
Overview of thrombolytic Agents:
These agents are used to dissolve blood clots which can block blood vessels. These agents are used to treat a variety of thromboembolic diseases, in which blood clots may be life-threatening. The thrombolytics break down the fibrin matrix within blood clots to restore blood flow.
They are used to treat conditions like acute myocardial ischemia (heart attacks), pulmonary embolism, and deep vein thrombosis. These agents are administered intravenously, and they can dissolve blood clots quickly. This could save lives and prevent long-term complications.
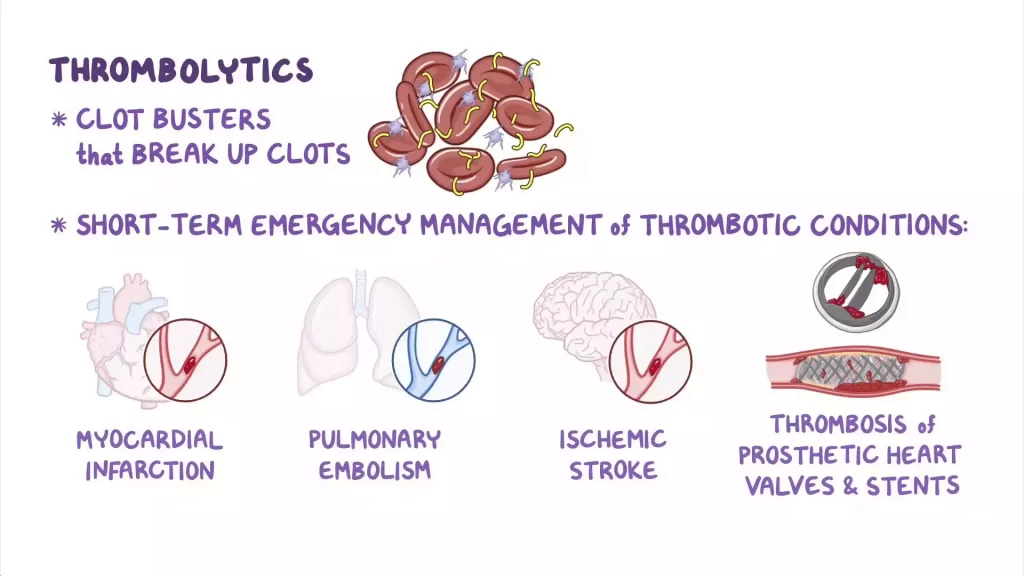
The risks of thrombolytic therapy, such as an increased bleeding risk, must be carefully balanced against its potential benefits.
The clinical situation, type of clot, and patient factors will determine the choice of a thrombolytic drug, such as Streptokinase. It is important for healthcare professionals that they understand the differences and mechanisms of action between these agents in order to make informed decisions.
Importance of understanding the differences between Streptokinase and Alteplase
For several reasons, it is vital to understand the differences between Streptokinase (Streptokinase) and Alteplase:
- Clinical decision-making: Healthcare providers need to make educated decisions about the thrombolytic agents to be used based on specific clinical scenarios and patient factors. Understanding the differences among these agents can help tailor treatment for optimal outcomes.
- Safety and Efficacy: The selection of a thrombolytic drug has a significant impact on efficacy. Understanding the mechanisms and risk profiles of Streptokinase versus Alteplase will allow for a more precise selection. This will minimize adverse effects and maximize clot dissolution.
- Time Sensitivity: When time is critical, such as in acute ischemic stroke and myocardial ischemia, rapid action by the thrombolytic is essential. Alteplase’s fibrin specificity allows it to act faster, which can improve treatment decisions.
- Patient Results: The use of the right thrombolytic can improve patient outcomes and reduce mortality and morbidity. Understanding the differences will ensure that patients get the best treatment possible for their condition.
- Bleeding Risk: Thrombolytic Therapy carries a bleeding risk. Streptokinase is associated with a higher bleeding risk because it’s non-specific. This can help guide monitoring and precautions to reduce this risk.
- Resource allocation: Healthcare systems and facilities must allocate resources efficiently. Understanding the differences allows hospitals to plan and allocate thrombolytics based on specific patient populations, clinical capabilities, and hospital needs.
- Research and Development: Understanding the differences between thrombolytic drugs can help guide research and development. It can be used to identify areas that need improvement in terms of safety and efficacy.
- Patient education: It is important to educate patients and their family members about the treatment that they receive. This will help them consent to it and adhere. Healthcare providers should explain the differences between their treatments to patients. This will increase trust.
The differences between Streptokinase (the active ingredient) and Alteplase (the inactive ingredient) are not just academically important, but they also have direct implications on patient care and the efficiency of healthcare systems. To make informed decisions that prioritize the safety and well-being of patients, healthcare professionals need to stay up-to-date on current guidelines and research.
Streptokinase and Alteplase in the comparison chart
Here’s a comparison chart summarizing the key differences between Streptokinase and Alteplase:
| Characteristic | Streptokinase | Alteplase (tPA) |
|---|---|---|
| Mechanism of Action | Non-specific; converts plasminogen to plasmin systemically | Fibrin-specific; activates fibrin-bound plasminogen |
| Indications | – Myocardial infarction (when other options are unavailable) | – Acute ischemic stroke within time window – Pulmonary embolism – Acute DVT (in some cases) |
| Dosage and Administration | Variable dosing, often single bolus injection | Weight-based dosing, bolus followed by infusion |
| Efficacy | Effective but non-specific, variable outcomes | Highly effective, targeted action on the clot |
| Speed of Action | Slower onset due to non-specificity | Faster onset due to fibrin specificity |
| Bleeding Risk | Higher bleeding risk due to non-specificity | Lower bleeding risk due to targeted action |
| Contraindications | – Active bleeding – Recent surgery or trauma – Known hypersensitivity |
– Active bleeding – Recent surgery or trauma – Known hypersensitivity |
| Precautions | – Renal or hepatic impairment – Coagulation disorders – Previous Streptokinase exposure |
– Renal or hepatic impairment – Coagulation disorders – Previous Alteplase exposure |
| Interactions | Interacts with anticoagulants, antiplatelet drugs, NSAIDs, and more | Interacts with anticoagulants, antiplatelet drugs, NSAIDs, and more |
| Clinical Guidelines | Used in specific situations per guidelines | First-line in acute ischemic stroke and PE per guidelines |
| Patient Education | Explain non-specificity and potential bleeding risk | Explain fibrin specificity and reduced bleeding risk |
| Availability | Available in some regions, less common | Widely available and preferred in many regions |
This chart gives a brief overview of the differences between Streptokinase and Alteplase. Clinical decisions must always be made based on current guidelines and the individual patient’s factors.
Background Information
The use of thrombolytics has revolutionized the treatment of thromboembolic diseases by allowing the dissolution of blood-clots which can block blood vessels. It is important for researchers and clinicians to understand their history and how they work.
- Historical Development:
- Researchers began investigating the possibility of removing blood clots in the early 20th century.
- Streptokinase was widely used in the middle of the 20th century. It is derived from a streptococcal bacterium. It was introduced to treat conditions such as myocardial ischemia.
- Due to their greater specificity and effectiveness, the development of newer agents such as Alteplase in the late 20th Century represented a significant advance in thrombolytic treatment.
- Mechanism of Action:
- Thrombolytics work by promoting plasminogen conversion into plasmin. This enzyme breaks down fibrin – the protein that makes up the structure of blood clots.
- The fibrinolysis mediated by Plasmin helps dissolve the clots and restore blood circulation in the affected vessel.
- Streptokinase, an early thrombolytic agent, is non-specific. It can activate plasminogen in both the clot as well as systemically.
- Alteplase is a modern thrombolytic that targets plasminogen activation within the clot. This reduces the risk of systemic bleeding.
- Clinical Significance:
- The role of thrombolytic therapy in treating acute thrombotic conditions, such as heart attacks, strokes with ischemic damage, pulmonary embolism, and deep vein thrombosis, is crucial.
- These agents are administered quickly and can save lives. They also reduce the effects of blood vessel blockage.
- The type of thrombotic symptom, the time since the onset of symptoms, and the medical history of the patient will all influence the choice of thrombolytic agents and treatment strategies.
- Safety Considerations:
- The increased bleeding risk associated with thrombolytic therapy must be assessed carefully in each patient.
- Patients who receive thrombolytics need to be closely monitored, as well as contraindications and possible interactions with other medications.
- The use of medical imaging and diagnostic techniques has improved the safety and selection of patients for thrombolytic treatment.
It’s crucial to understand the differences between Streptokinase (a thrombolytic agent) and Alteplase (a thrombolytic agent), to make informed decisions about their roles in clinical practice.
Mechanism of Action
Mechanisms of Action for Streptokinase & Alteplase:
Both Streptokinase (also known as Alteplase) and Alteplase, which are used to dissolve blood clots by thrombolysis, have different mechanisms of action.
Streptokinase:
- Plasminogen activation: Streptokinase is a non-specific agent that acts as a thrombolytic. It does not directly bind to fibrin, which is the main component in blood clots.
- Systemic activation: When administered intravenously Streptokinase circulates through the entire body. It activates the plasminogen both in the clot and in systemic circulation.
- Formation of Plasmin: Streptokinase converts plasminogen into active plasmin by forming a complex in the blood.
- Fibrinolysis: Plasmin breaks down fibrin (the mesh-like structure that forms blood clots), leading to the dissolution of these clots.
- Non-Fibrin Specificity: Streptokinase is effective in dissolving clots of various types, but it also increases the chance of systemic bleeding.
Alteplase (tissue plasminogen activator – tPA):
- Fibrin Specificity: Alteplase, a more fibrin-specific thrombolytic drug. It binds to fibrin in the blood clot.
- Activation of Plasminogen: Alteplase is primarily used to activate the plasminogen bound to fibrin in a thrombus.
- Localized action: Alteplase is fibrin-specific, meaning that it activates plasmin primarily within the clot. This reduces the risk of bleeding systemically.
- Fibrinolysis: Alteplase generates a plasmin that targets the fibrin strands in the clot. This leads to the clot being disintegrated while sparing healthy tissue.
- Improved Safety: Alteplase is a safer alternative to Streptokinase due to its targeted action.
Streptokinase activates the plasminogen in both the clot as well as systemically. This leads to non-specific dissolution of the clot, which increases the risk of bleeding.
Alteplase, however, binds to fibrin in the clot. This leads to targeted fibrinolysis and reduces systemic bleeding risks. It is therefore preferred for certain clinical scenarios such as acute stroke or pulmonary embolism.
The choice of the appropriate thrombolytic drug depends on the clinical condition, the patient’s factors, and the desired balance between safety and efficacy.
Indications
Streptokinase Indications:
Streptokinase was used to treat a variety of thrombotic conditions. However, its use is less common now that fibrin-specific thrombolytics like Alteplase have been developed. It may be used in some situations.
- Acute myocardial infarction (Heart attack):
- When more fibrin-specific drugs like Alteplase and primary percutaneous coronary interventions (PCI) such as PCI are not available, or contraindicated, then streptokinase may be an alternative option to reperfusion therapy for patients with ST-segment elevation myocardial ischemia (STEMI).
- Deep Vein Thrombosis (DVT):
- When other options are unavailable, streptokinase can be used to treat acute DVT.
Alteplase (tPA):
Alteplase, a fibrin-specific agent, is used in a variety of clinical situations.
- Acute Ischemic Stroke:
- Alteplase can be used as a first-line treatment for acute strokes if administered within a certain time frame (typically 4.5 hours after the onset of symptoms) and only if contraindications have been excluded.
- This product helps to restore blood flow in the brain and reduce neurological damage.
- Pulmonary Embolism:
- Alteplase can be used to treat acute, life-threatening, pulmonary embolism in patients with hemodynamic instability.
- Acute Massive Deep Vein Thrombosis (DVT):
- Alteplase is effective in treating massive DVTs, particularly when they are associated with symptoms or risk of pulmonary embolism.
- Coronary Artery Thrombosis:
- Alteplase is an alternative to primary PCI for acute myocardial ischemia when timely PCI cannot be performed, as in remote areas.
The selection of the right thrombolytic and its indications must be made based on clinical conditions, patient factors (including any contraindications), and the treatment window. When applicable, the choice between Streptokinase or Alteplase depends on both the clinical context as well as available treatment options.
Dosage and Administration
Dosage and Administration of Streptokinase :
Streptokinase dosages and administration can be adjusted depending on the thrombotic condition, and the protocols of the healthcare facility. It is usually administered intravenously.
- Acute myocardial infarction (Heart attack):
- Streptokinase can be administered in a single injection.
- The dose may vary, but it is usually around 1.5 million units over 30-60 minutes.
- In some cases, additional doses or infusions might be considered.
- Deep Vein Thrombosis (DVT):
- DVT dosage and administration can be varied. The infusion is usually given continuously over several hours.
- The severity of DVT, the condition of the patient, and the protocol and dosage used will determine the specific protocols and dosages.
- Dosing considerations:
- The dosage can be adjusted depending on the weight of the patient and their clinical presentation.
- A healthcare professional should decide whether or not to administer Streptokinase, and what dosage regimen is appropriate, based on a patient’s medical condition and clinical guidelines.
Dosage and Administration of Alteplase tPA:
Alteplase comes with specific guidelines for administration and dosage, especially in the treatment of acute ischemic strokes, pulmonary embolisms, and acute coronary symptoms.
- Acute Ischemic Stroke:
- The dosage recommended for acute ischemic stroke is usually calculated using the weight of the patient, with a prescribed maximum dose.
- The initial bolus is followed by an hour-long infusion.
- The administration is time-sensitive and should begin as soon as possible, within the time frame approved. This time period is typically 4.5 hours after the onset of symptoms.
- Pulmonary Embolism:
- Alteplase is usually administered by a bolus followed by a continuous infusion.
- The dose and the administration may differ depending on the weight of the patient and the severity level of PE.
- Acute Coronary Syndromes:
- Alteplase has a lower use rate for acute coronary syndromes than primary PCI.
- The dosage and administration of the drug will depend on clinical scenarios and institutional protocols.
- Considerations for Dosing:
- Alteplase should be administered in accordance with established protocols and guidelines.
- To balance the benefits of dissolving clots with the risks of bleeding, it is important to dose accurately.
When using Streptokinase and Alteplase, it is important that healthcare professionals consult their facility’s specific guidelines and protocols and follow the recommended dosages and procedures.
When determining an appropriate thrombolytic treatment, it is important to consider patient factors such as contraindications, time since the onset of symptoms, and other factors.
Efficacy and Speed of Action
Streptokinase and Alteplase: Efficacy, Speed of Action
In clinical practice, the efficacy and rapidity of thrombolytics are important factors. They determine how quickly and effectively they dissolve blood clots. These aspects are different between Streptokinase, and Alteplase due to their unique mechanisms of action.
Streptokinase:
- Efficacy:
- Streptokinase promotes clot dissolution but is not specific in its actions. It activates the plasminogen within and outside of the clot.
- Streptokinase’s non-specificity may cause a more widespread fibrinolysis and increase the risk of bleeding complications.
- The effectiveness of this treatment depends on the clinical situation, the age, and individual characteristics of the patient.
- Speed of Action:
- Streptokinase has a generally slower onset of effect compared to fibrin-specific agents such as Alteplase.
- Streptokinase may require more time to dissolve clots due to the need to produce plasmin in all parts of the circulatory system.
Alteplase tPA:
- Efficacy:
- Alteplase’s fibrin-specific effect makes it highly effective in promoting clot dissolution. It activates fibrin-bound plasminogen within the clot and spares systemic circulation.
- This targeted fibrinolysis increases the efficacy of the agent while minimizing systemic bleeding.
- Speed of Action:
- Alteplase is more rapid than Streptokinase. Its fibrin specificity allows it to initiate fibrinolysis faster at the site where the clot is.
- Alteplase is an excellent choice for clinical situations such as acute ischemic stroke when time is critical. It can save brain tissue by administering it within the recommended window of time.
Alteplase’s fibrin-specific action is considered to be more effective and faster than Streptokinase. The targeted approach of Alteplase allows for a more rapid dissolution while reducing systemic bleeding complications.
The non-specificity of streptokinase may cause a slower onset and higher bleeding risks, even though it is still effective in some situations. When choosing between thrombolytics, it is important to consider the patient’s condition, their eligibility, and the desired balance of efficacy and security.
Side Effects and Adverse Reactions
Adverse reactions and Side effects of Streptokinase:
Like other thrombolytics, streptokinase can have a variety of adverse effects, some of them serious. When using this medication, it’s important to balance the benefits and risks of clot removal.
Side Effects of Common Drugs:
- Bleeding: The most common Streptokinase side effect is bleeding. It can be a minor bleeding of the nose or gums, or it could be a more serious bleeding such as gastrointestinal hemorrhage or hematuria.
Less common side effects: Allergic reactions: Some people may have allergic reactions such as hives, rash, or itching. More severe allergic reactions, like anaphylaxis, can also occur.
- Fever & Chills: Flu-like symptoms including fever & chills can occur after Streptokinase treatment.
- Vomiting and Nausea: These symptoms are less frequent but still possible.
- Hypertension: A fall in blood pressure can cause dizziness and fainting.
Severe Adverse Reactions:
Intracranial Hemorrhage: This is a serious and potentially life-threatening side effect associated with thrombolytic treatment. It can cause stroke-like symptoms or altered mental status.
- Significant Blood Loss: Severe bleeding can occur in various parts of the body, such as the gastrointestinal tract and genitourinary systems.
- Allergic Anaphylaxis: In rare cases, anaphylactic reactions may occur. These include difficulty breathing, swelling, and a decrease in blood pressure.
Compare with Alteplase tPA:
Streptokinase is associated with a greater risk of bleeding compared to Alteplase due to its nonspecific action on activating plasminogen, which may lead to a more widespread fibrinolysis. Alteplase is fibrin-specific, which allows it to target the clot and reduce the risk of systemic events.
Before administering Streptokinase, it is important that healthcare professionals carefully evaluate patients to determine if there are any contraindications or risk factors of bleeding. It is also important to monitor patients closely during and after the treatment in order to detect any complications or adverse reactions.
When choosing a thrombolytic drug, it is important to consider both the efficacy of the agent and its safety profile. This includes the side effects and adverse reactions that may occur.
Contraindications and Precautions
Contraindications, Precautions, and Streptokinase:
Healthcare professionals should evaluate the patient for contraindications before administering Streptokinase. They should also take precautions to reduce any risks associated with using this thrombolytic drug.
Contraindications:
- Active bleeding: Streptokinase should not be used in patients who have active bleeding disorders. This includes gastrointestinal bleeding, intracranial bleeding, or bleeding at other sites.
- Recent Trauma or Surgery: Patients with recent major surgery or trauma are usually contraindicated from Streptokinase because of the increased bleeding risk.
- Hypersensitivity: Patients with known hypersensitivity to Streptokinase, or any component of it, should not be given this medication.
- Stroke History: Streptokinase is not recommended for patients with a past history of hemorrhagic or other bleeding disorders.
- Severe, Uncontrolled Hypertension: Individuals with uncontrolled severe hypertension (high blood pressure) are at an increased risk of bleeding complications if Streptokinase is used.
Precautions:
- Recent Invasive Procedures: Patients with recent invasive procedures such as arterial puncture and lumbar puncture may have a greater risk of bleeding complications if treated with Streptokinase.
- Previous Streptokinase Exposition: Patients who have previously been exposed to Streptokinase are at a higher risk of developing antibodies that could reduce the effectiveness of the drug if it is used again.
- Lactation and Pregnancy: Streptokinase should only be used with extreme caution during pregnancy and breastfeeding. Alternative treatments may be safer for pregnant women.
- Age: Older patients are more likely to experience bleeding complications, and they should be closely monitored if Streptokinase is used.
- Renal or Hepatic Impairment: Patients with severe renal or liver impairment may need to adjust their doses since Streptokinase leaves the body via these organs.
- Coagulation disorders: Patients who have underlying coagulation problems or bleeding tendencies, should be closely watched for signs of bleeding.
Streptokinase contraindications, precautions, and institutional protocols may differ. A qualified healthcare professional should make the decision to use Streptokinase after thoroughly assessing the patient’s medical background and risk factors.
Streptokinase patients should also be closely monitored throughout and after the treatment in order to detect and promptly manage any adverse effects or complications.
Interactions with Other Medications
Interactions between Streptokinase or Alteplase and Other Medicines:
When prescribing and administering these thrombolytic drugs, healthcare professionals need to be aware of the interactions.
Interactions between Streptokinase and:
- Anticoagulants: Concurrent use with Streptokinase of anticoagulants, such as heparin or warfarin, can increase bleeding risk.
- Antiplatelet Drugs: Aspirin, Clopidogrel or other antiplatelet agents may increase the risk of bleeding if used with Streptokinase. A careful assessment of bleeding risks is required.
- Thrombolytics: The use of multiple thrombolytics simultaneously is generally not recommended because it increases the risk of bleeding complications.
Interactions of Alteplase with tPA:
- Alteplase and Anticoagulants: Alteplase may interact with anticoagulants increasing bleeding risk. Alteplase should only be combined with anticoagulant treatment with extreme caution.
- Antiplatelet Agents: Similar to Streptokinase use of Alteplase with antiplatelet agents can increase the risk of bleeding. When deciding whether to use both agents, it is important to consider the risk of bleeding.
- Thrombolytics: The simultaneous use of several thrombolytics, including Alteplase is generally discouraged because of the increased risk of bleeding.
- Hormone Replacement Therapy and Oral Contraceptives: Combining estrogen-containing medications with Alteplase is not recommended.
- Alternatives to Alteplase: Patients should discuss the use of herbal supplements with their healthcare provider.
- NSAIDs: NSAIDs Alteplase and NSAIDs can increase bleeding risk, especially gastrointestinal bleeding. Avoid or use these drugs with caution.
Before administering Streptokinase and Alteplase, healthcare professionals should review the complete medication profile of a patient, including herbal supplements, over-the-counter medications, and prescription drugs. This will allow them to identify any potential drug interactions.
To minimize the risk of drug interactions, it may be necessary for the patient to be closely monitored and to make appropriate changes to their treatment plan.
Current Clinical Guidelines
Since my last update of knowledge in September 2021 I do not have access to any specific clinical guidelines after that date. As new evidence and medical practices change, clinical guidelines for the use of thrombolytic drugs such as Streptokinase or Alteplase can also evolve.
To make an informed decision about the use of these medications, it is important to consult the most recent clinical guidelines, which are available from reliable sources such as medical associations or government agencies.
Clinical guidelines for thrombolytic treatment and the use of Streptokinase or Alteplase are available from:
- American College of Cardiology: ACC offers guidelines for the management of cardiovascular disease, including myocardial ischemia and thrombolytic treatment.
- American Heart Association: AHA provides guidelines for treating cardiovascular diseases including stroke and acute coronary syndromes.
- The European Society of Cardiology: ESC has published guidelines for the management of cardiovascular disease, including recommendations regarding thrombolytic treatment.
- National Institute for Health and Care Excellence: In the UK, NICE produces guidelines for various medical treatments, including thrombolytic drugs.
- World Health Organization: WHO can provide global guidelines on the treatment of specific medical conditions including thrombotic disorders.
- Local Health Authority: Regional and national health authorities often release guidelines that are specific to their healthcare systems or populations.
Please consult the official websites of these organizations to access the latest and most relevant clinical guidelines or the guidelines published locally by your health authority.
To ensure that they are following the most recent recommendations and evidence-based practices, healthcare professionals can also seek guidance from local experts or institutions.
Conclusion
Alteplase and Streptokinase are two thrombolytics with different mechanisms of action, indications, and safety profiles. Alteplase, which is fibrin-specific, is faster and more targeted but carries less bleeding risk. Streptokinase, on the other hand, is non-specific and has a higher bleeding risk.
When choosing between these agents, it is important to consider factors such as the clinical condition, the patient, and the balance of efficacy and security. When using these medications, healthcare professionals should adhere to clinical guidelines, and consider drug interactions, contraindications, and precautions.
